Data Solutions for Healthcare Plans & Payers
Accelerate credentialing processes and enhance data integrity with Verisys’ healthcare payer solutions, data-rich tools, and longitudinal provider profiles.
Verisys offers efficient healthcare payer solutions as your secure and trusted source for provider data that mitigates risk, lowers operational costs, and streamlines healthcare administration functions. These solutions ensure quality care and optimal health outcomes.
The Stats That Matter
Providers Monitored Annually
Payer Clients
Credentialing Events Annually
Empowering Health Plans with Unmatched Data Precision and Scalable Credentialing Solutions.
Here’s Verisys delivers unparalleled value for health plans:
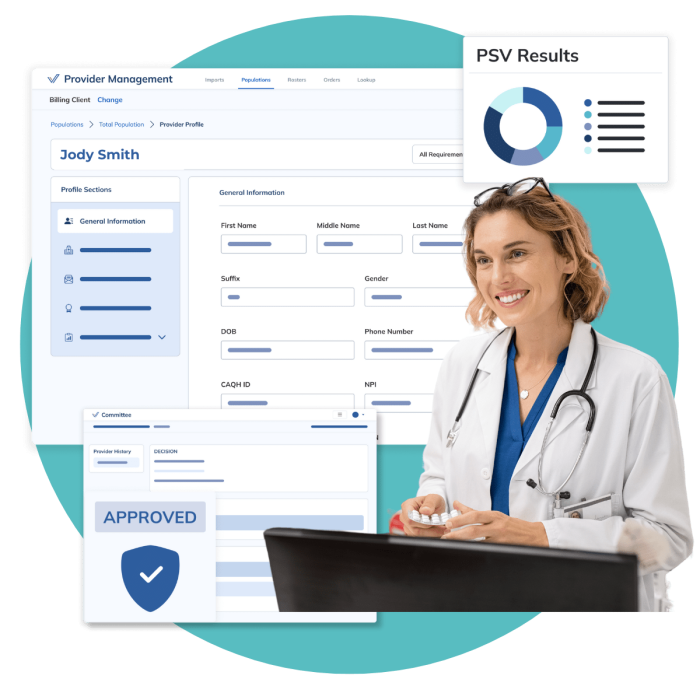
Credentialing
Verisys is the largest outsourced healthcare credentialing provider in the market today and the only player with the workflow expertise and in-house database (i.e., FACIS®) to efficiently serve the end-to-end needs of large healthcare clients.
For three decades, Verisys has supported client components of network management to ensure regulatory compliance and enable payors to keep an up-to-date provider network. Our credentialing solutions are trusted by healthcare organizations nationwide to support compliance, optimize provider relationships, and transform care management.
Verisys credentialing is the only NCQA and URAC accredited solution to maintain the industry’s highest data and compliance standards.
Our healthcare payer solutions allow you to conduct provider credentialing searches efficiently, seamlessly integrate primary-source data into your current processes, and improve workflow efficiency—all while reducing risk and ensuring better care.
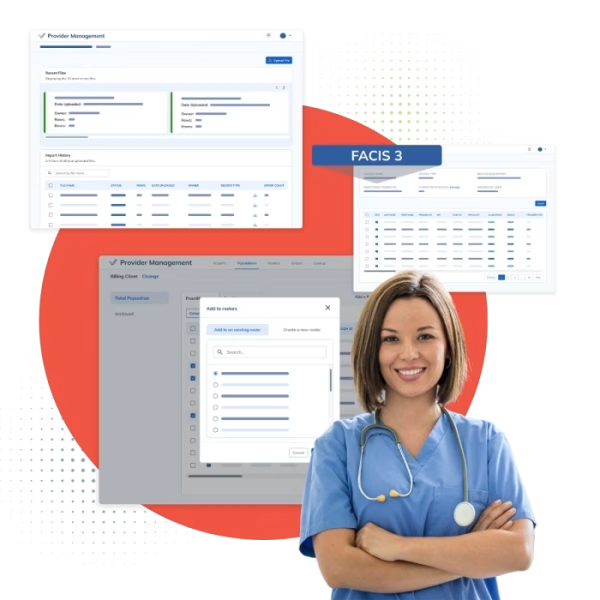
FACIS: The Gold Standard in Sanction Monitoring
When it comes to keeping customers and patients safe, you need the gold standard.
FACIS is the industry’s most comprehensive database consisting of primary content from federal and state sources for exclusions, sanctions, debarments, disciplinary actions, and adverse events against healthcare professionals and entities for all 868 taxonomies and all 56 U.S. states and jurisdictions. A database of over 10 million records from 3,500 primary sources on provider exclusions, sanctions, and adverse events, FACIS delivers 360-degree transparency on providers, staff, and entities for the organizations who hire, credential, refer, and reimburse for healthcare delivery.
Licensing
Faster healthcare license verification to accelerate efficiency and reduce fraud and waste.
Provide a point-in-time license verification of a professional license number, including status, issue and expiration date, primary source information, and any disciplinary action (current or historical). Search aliases are provided for each practitioner as part of the search criteria and verification process.

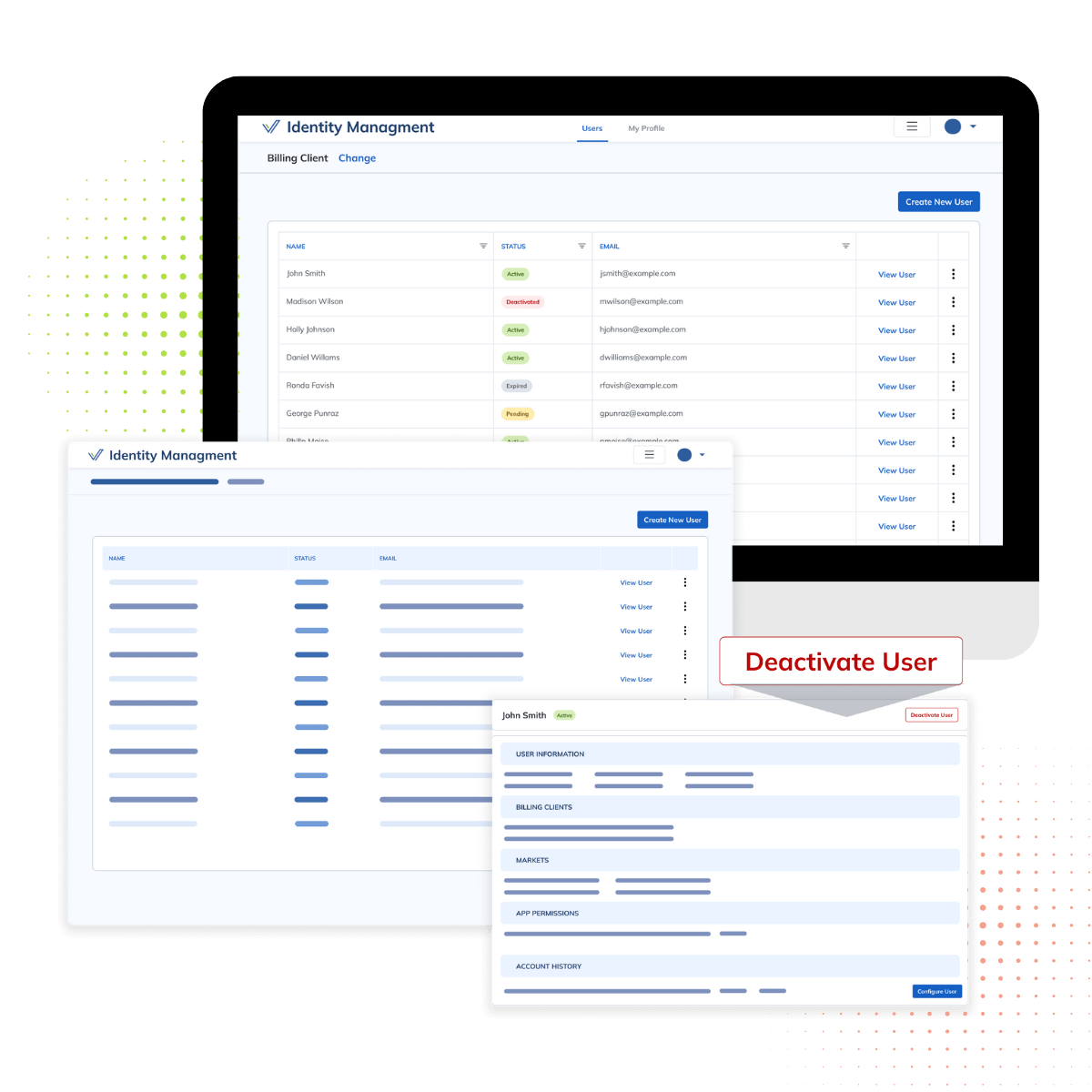
Workforce Management
Verisys’ Provider Directory Management Solutions transform often flawed provider data into comprehensive, customizable directories that integrate seamlessly with your member portal. We display intricate networks how you want your members to see them, highlighting and tiering network providers just for them — including telemedicine providers.
By delivering relevant, actionable information, consumers can make informed decisions leading to better outcomes—one of healthcare reform’s primary goals.
By offering a more comprehensive, integrated provider search platform, you can keep current members satisfied and engaged while attracting new customers who want to strengthen member engagement.
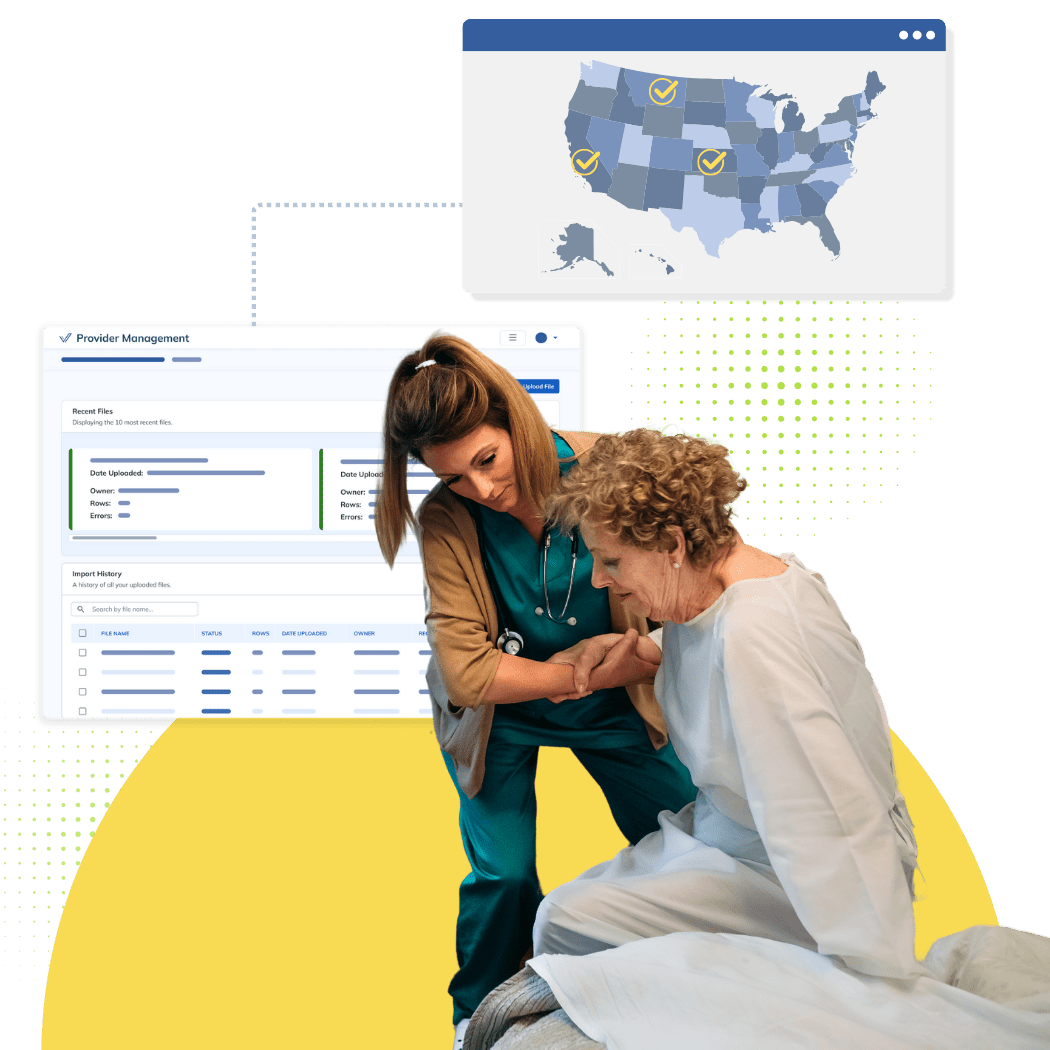
True Monitoring
The best way to ensure all practitioner licenses remain in good standing is through continuous healthcare compliance monitoring for licenses.
Continuously monitoring your population adds a layer of security and makes ongoing compliance with regulations set by standard-setting bodies possible. To stay in compliance with federal and state regulations and to keep patients safe, it’s vital for hospitals and health systems to monitor the licenses of their practitioners for new information that may prevent a physician from practicing. If a practitioner’s license is invalid, suspended, or expired, or if restrictions are placed on a license, healthcare organizations must take steps to halt the treatment of patients until the practitioner gets his license back in good standing.

Streamline network administration with our configurable payer credentialing solutions and up-to-the-minute provider directories powered by accurate, verified data.
READY TO STREAMLINE Your Compliance?
Let Verisys optimize payer network functions including credentialing, employee monitoring and provider network data augmentation through technology and data.
Do more with Verisys
Enhance your compliance and operational processes with solutions tailored to your needs.
FACIS®

License Verification

Credentialing

Pre to Post Hire Screening
Workforce Management

True Monitoring
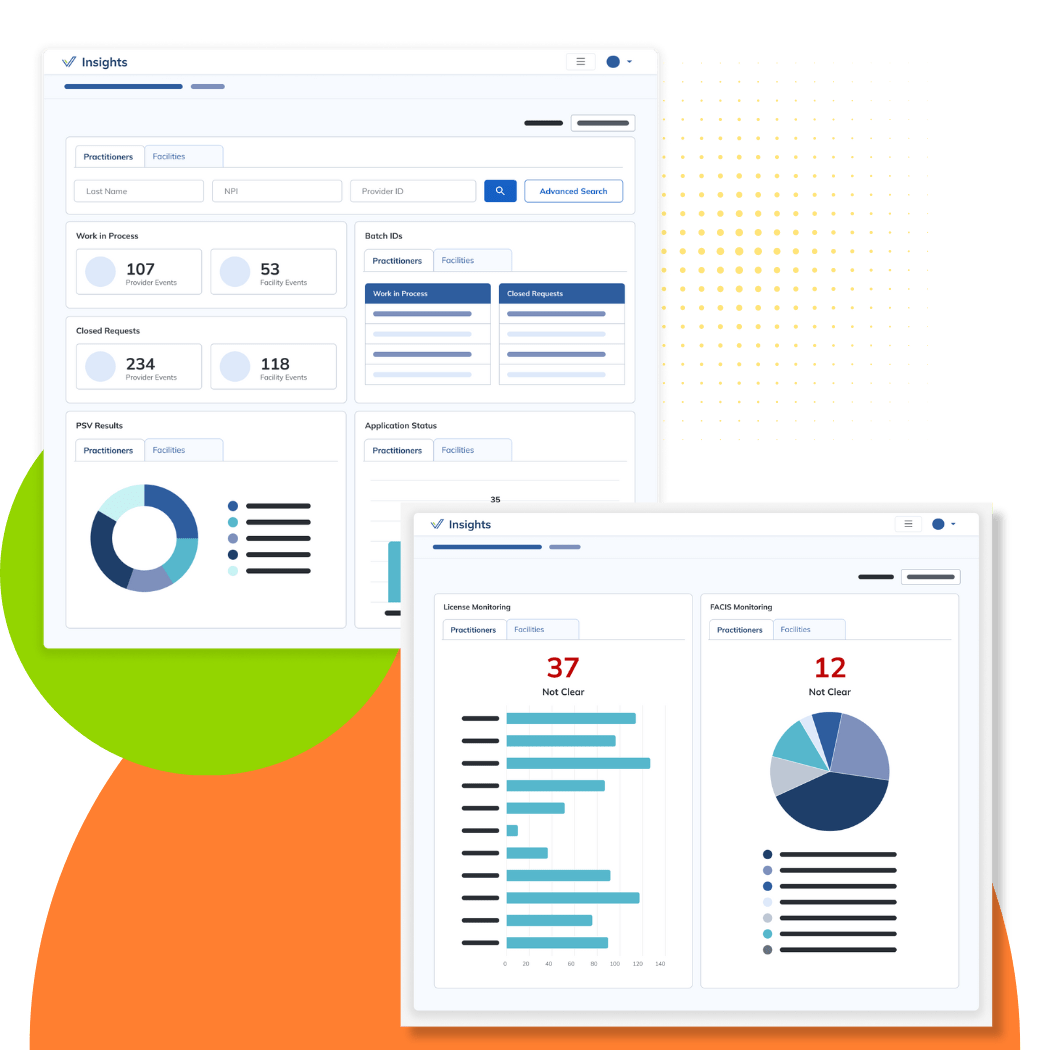
Profiles Dataset
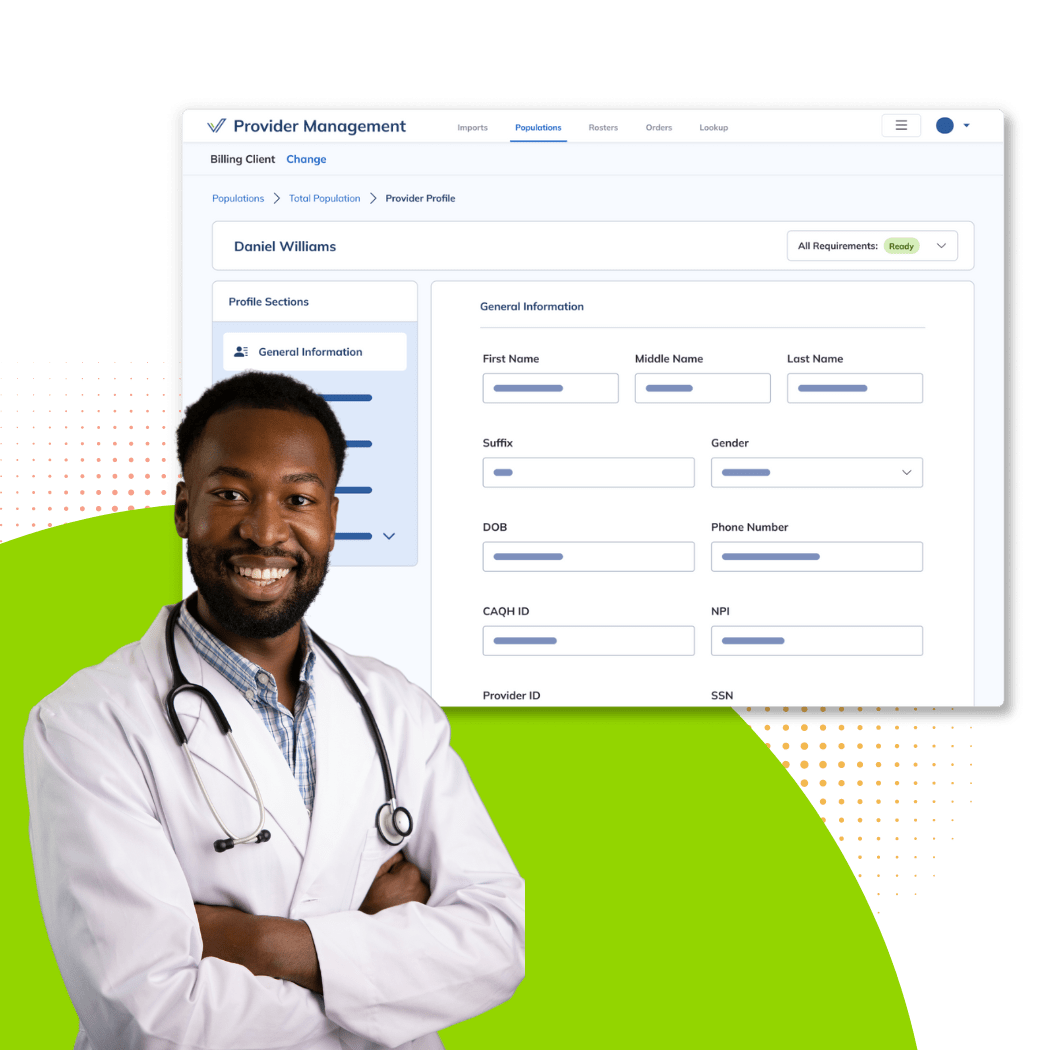
Unified API















