Monitor OFAC+ for Complete Compliance
Verisys’ OFAC+, a proprietary aggregated dataset, provides data related to anti-money laundering screening, a requirement under various federal laws and regulations. Automated systems reduce the potential for errors, enable more consistent monitoring, and lighten the administrative load.
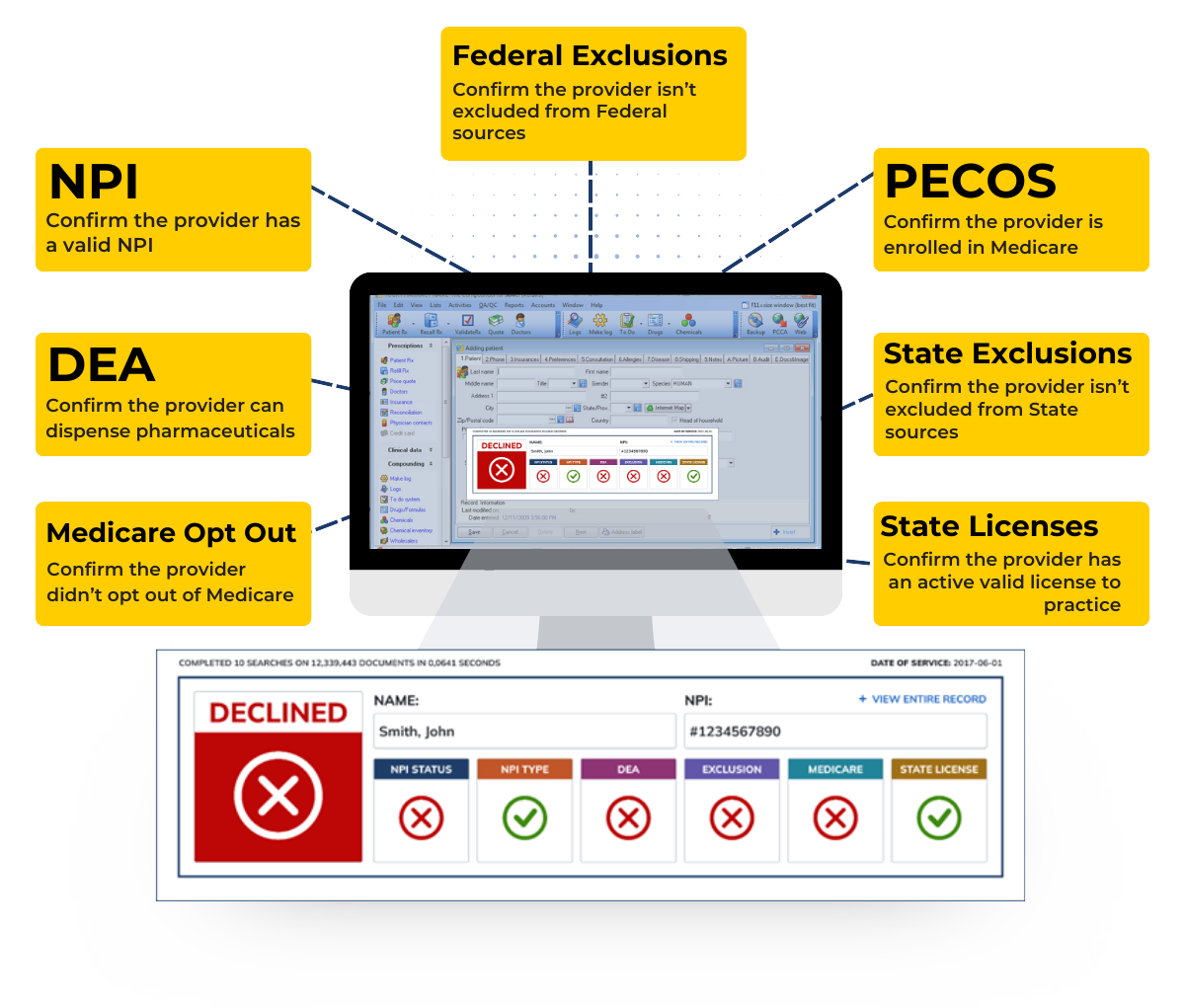
Eligibility is designed to reduce organizational risk and improve operations for healthcare organizations.
Initial use cases for Eligibility include:
- Pre-Enrollment screening to ensure a provider is eligible to see patients
- Point of prescription fill eligibility screening to ensure your eligibility to provide medicine
- Eligibility screening at point of claim payment to help reduce fraud, waste, and abuse.
- Underwriting risk assessment for providers and entities
Eligibility is designed to reduce organizational risk and improve operations for healthcare organizations.

Eligibility was designed with the pharmacy market in mind. Over the past several years, the role of the pharmacist has greatly expanded and the background screening needs have evolved with the role. Eligibility was created to help solve common pharmacy pain points:
- Real time confirmation of prescription fills and immediate alerts to changes in status
- Real time review of prescribing provider status and alerts to potential issues
Eligibility was designed with the pharmaceutical and life science organizations in mind. Verisys is state and federal regulation compliance experts curating the most comprehensive provider data. Eligibility was created to help solve common pain points:
- Real time transactional pre-employment screening
- Real time review of prescribing provider status and alerts to potential issues


Eligibility was designed with the payer market in mind helping to solve common pain points:
- Real time confirmation of eligibility for pre-enrollment screening
- Real time confirmation of eligibility screen at point of claim payment
- Real time review of underwriting risk assessment
%
of Individuals Submitted are Identified
Providers Monitored Annually
%
Verification Accuracy
“The verification process takes too long and is too rigid. We want to break apart the process to be more dynamic and to help save organizations time and money.”
Eligibility is an easy to implement and integrate solution.

- Seamless API integration into existing organizational tech stack to streamline reporting
- Pre-schedule eligibility screening to minimize potential missed screenings
- Minimize the need for additional data to be provided from your organization














