Hospital Credentialing Services
Single Source for Complete Health System Compliance
Verisys helps hospitals and health systems mitigate risk, reduce operational costs, and streamline compliance workflows so they can focus on delivering quality care and achieving better patient outcomes.
Enterprise Compliance Without Compromise: Credentialing, Sanctions & Exclusions Monitoring forHealthcare Systems
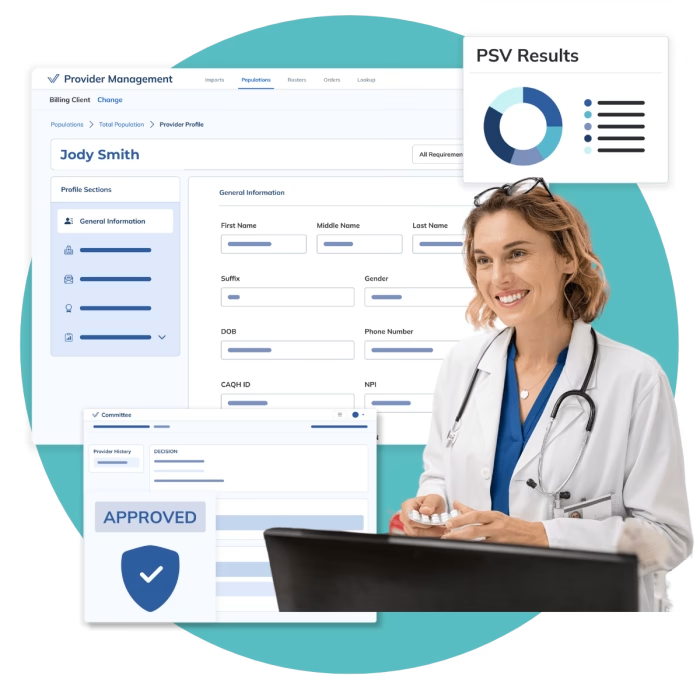
Verisys’ comprehensive data solutions enable hospitals and health systems to streamline and automate exclusion screening, license verification, provider credentialing, and continuous monitoring of your workforce.
Verisys’ data solutions alleviate the administrative burden on your staff while simplifying and expediting compliance processes. Automate provider sanctions, exclusions, and adverse events screening with FACIS. Supplement FACIS by monitoring providers against:
- NPI
- Sex Offender & Abuse registries
- DEA & CDS registries
Continuous monitoring will automatically alert you to any new findings for a provider. Hospital staff, practitioners, and vendors can be added to the monitoring service.
It can be challenging to monitor license, registration, and certification status and track expiration dates. To ensure ongoing compliance, implement a solution built for hospitals and health systems that monitors for changes in license status and provides pre-expiration notifications.
Our credentialing services reduce administrative redundancy and ensure compliance with quality standards and industry regulations.
Verisys is your secure, efficient, and trusted source for provider data that mitigates risk, lowers operational costs, and streamlines network administration functions so you can focus on delivering quality care and achieving optimal outcomes.
Our Stats
With over 30 years serving and partnering with some of the largest health systems and provider organizations, we are experts in data.
Provider Records
With tens of millions of records, Verisys stands out from competitors by providing more comprehensive, actionable data that keeps patients and organizations safe.
Primary Sources Actively Monitored
The most accuracy provider data on the market.
%
Verification Accuracy
Verisys breadth of data and accuracy is why large organizations trust Verisys with their compliance needs.
Empowering Health Systems with Unmatched Data and Scalable Compliance Solutions
Pre-Hire Screening
Screen and verify all licensed and non-licensed candidates against critical data sets, including FACIS, licensing boards, Medicare opt-out, NPDB, preclusion lists, sex offender and abuse registries, and more.
Compliance Monitoring
Protect your patients, providers, and organizations from compliance risks with continuous compliance monitoring. Verisys automated alerts notify you of any new provider finding, including preliminary and leading indicators, ensuring your organization has the full picture.
Credentialing
NCQA certified & URAC accredited compliant credentialing for all providers. Verisys is the largest CVO provider. All dynamic and expirable credential types can be enrolled in ongoing monitoring for changes in status and expiration/renewal.
Payment Integrity Solutions
Real-time confirmation of provider and prescriber eligibility to prevent false claims submissions and non-payment due to provider ineligibility. Receive real-time, continuous confirmation for exclusions, licensure, DEA, Medicare Opt-Out, and PECOS enrollment.
Why Leading Health Systems Choose Verisys
A Proven Partner in Compliance, Credentialing, and Workforce Integrity
Hospitals and health systems require more than just a dashboard—they need a trusted partner to help ensure regulatory compliance, protect patient safety, and streamline operations. Verisys delivers unmatched depth, accuracy, and responsiveness in provider and workforce data, making us the compliance engine behind some of the most respected healthcare organizations in the country.
The Golden Record of Provider Data
Verisys uncovers 30% more provider data than other solutions, offering a more complete and accurate picture to support compliance and operational efficiency.
Real-Time Alerts and Seamless Integration
Our system delivers instant notifications for exclusions, sanctions, and licensure changes—so your compliance team can act immediately.
Better Data, Smarter Decisions, Improved Outcomes
Data is delivered through a unified API or web portal, reducing administrative burden and supporting timely decision-making.
Trusted Security and Industry Standards
Verisys is SOC2 certified and FCRA-audited, ensuring secure and compliant handling of sensitive provider data.

Who
Who We Empower in Health Systems
Medical Staff & Credentialing Teams
- Eliminate manual verification and streamline credentialing workflows
- Reduce provider onboarding time and increase operational efficiency
- Accelerate provider onboarding while maintaining compliance
Compliance & Risk Management Leaders
- Proactively monitor sanctions and exclusions
- Protect your system from non-compliant or fraudulent providers
- Ensure readiness for audits and adherence to regulatory standards
- Centralize all provider and staff compliance data in one place
Human Resources and Workforce Screening Teams
- Improve compliance with continuous workforce screening
- Ensure all employees meet regulatory and credentialing requirements
- Conduct comprehensive background and exclusion checks
- Reduce liability and protect patients through smarter hiring

Compliance Resources for Hospitals and Health Systems
Ready to Elevate Your Compliance?
Contact us today to learn more about Verisys healthcare compliance solutions and how we can integrate our Gold Standard data to meet your unique needs.




















